- ENGLISH/ITALIANO
- About Us
- Courses
- Teaching staff
- Research
- Enrolment
- Student services
- Faq and Contact
- News
- Vacancies
- Work with us
Project: “Progress of rehabilitation: physiological, psychological and neuroimaging measurements of factors that predispose, cause and perpetuate post-traumatic vertigo”.
Project manager: Prof. Iole Indovina
For studies on patients with persistent subjective vertigo, a 4-year funding (2018-2022) was allocated from the US Department of Defense (Congressionally Directed Medical Research Program W81XWH1810760 PT170028). The research project involves the collaboration between UniCamillus, the Mayo Clinic of Rochester (project leader), the University College of London, the Santa Lucia Foundation IRCCS of Rome and the University of Rome “Tor Vergata”.
 The project – Persistent subjective vertigo (dizziness)
The project – Persistent subjective vertigo (dizziness)
The research focuses on the study of brain perception and cognitive mechanisms through functional magnetic resonance imaging (fMRI).
– Visual-vestibular perception
– Coding of the internal gravity model
– Neural coding of navigation in three-dimensional space
– Alteration of such mechanisms in chronic vestibular patients
– Interaction between pathological vestibular conditions and anxiety
Persistent subjective vertigo (dizziness)
 Persistent subjective vertigo consists in the feeling of jolting or swinging, feeling weak, unstable or having the impression of “not having the ground under your feet” or even falling to the ground (without ever really falling). Subjective vertigo therefore concerns a feeling of movement and instability of the person (therefore it does not refer to the external environment but to oneself). The English term for this complex symptomatology is dizziness. Subjective vertigo is distinguished from the objective classical vertigo which is instead the feeling of seeing the space around moving or spinning (this objective vertigo is often associated with strong nausea and vomiting while subjective vertigo is not). This sight or being in the situations in the picture is particularly annoying for those suffering from subjective vertigo.
Persistent subjective vertigo consists in the feeling of jolting or swinging, feeling weak, unstable or having the impression of “not having the ground under your feet” or even falling to the ground (without ever really falling). Subjective vertigo therefore concerns a feeling of movement and instability of the person (therefore it does not refer to the external environment but to oneself). The English term for this complex symptomatology is dizziness. Subjective vertigo is distinguished from the objective classical vertigo which is instead the feeling of seeing the space around moving or spinning (this objective vertigo is often associated with strong nausea and vomiting while subjective vertigo is not). This sight or being in the situations in the picture is particularly annoying for those suffering from subjective vertigo.
Frequent episodes of subjective vertigo, or continuous subjective (persistent) vertigo can have a very negative impact on the quality of life, even though they do not represent a danger of imminent death.
The treatments for subjective vertigo depend on the underlying specific causes.
To be defined as persistent, subjective vertigo must last for at least 3 months, not necessarily continuous. It must also be present for most days, although not necessarily every day.
Subjects with persistent subjective vertigo describe the following feelings:
– A feeling of themselves moving, of postural instability and of unsteady walk (feeling of falling to the ground without ever falling)
– “Light Head” or “Heavy Head”
– Instability and loss of balance
– Feeling of floating
These sensations can be triggered or exacerbated by walking, standing upright or moving the head. In addition, they can increase in very crowded or full places or in environments such as those shown in the figure. Some people often feel subjective vertigo when they walk among the crowded shelves of a supermarket.
The typical events that can trigger (in predisposed subjects) the persistent subjective vertigo are:
– head trauma (mild, moderate or even severe), typically after car or domestic or other accidents in which one hit his head and lost consciousness for a few seconds or even minutes or hours;
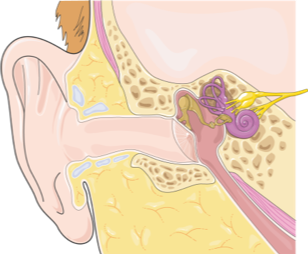
– vestibular neuritis or benign paroxysmal positional vertigo (BPPV). These otorhinolaryngological diseases (that is, those that concern the inner ear) are a frequent cause of classical objective vertigo that typically resolves itself spontaneously or after treatment in a few weeks. In most cases the patient gets back to normal and no longer feels any vertigo-inducing disorder. However, there are some predisposed subjects in whom the acute event of vestibular neuritis or BPPV triggers a chronic and persistent subjective vertigo;
– the symptoms of persistent subjective vertigo are clearly different from those of vestibular neuritis or BPPV as explained above but there is a clear causal relationship between the two events (e.g BPPB before and subjective vertigo then);
– panic attacks, hypotension (low blood pressure), generalized anxiety, cardiac arrhythmia (abnormalities of the heartbeat);
– migraine, other forms of acute or chronic headache.
As mentioned above, one of the most important features of persistent subjective vertigo is that it is chronic, that is, it persists even after the triggering episode has resolved
Risk factors
Factors that could increase the risk of developing persistent subjective vertigo include:
Indovina, I., Riccelli, R., Chiarella, G., Petrolo, C., Augimeri, A., Giofrè, L., Lacquaniti, F., Staab, J.P., Passamonti, L., 2015. Role of the Insula and Vestibular System in Patients with Chronic Subjective Dizziness: An fMRI Study Using Sound-Evoked Vestibular Stimulation. Front. Behav. Neurosci. 9, 334. https://doi.org/10.3389/fnbeh.2015.00334
Indovina, I., Riccelli, R., Staab, J.P., Lacquaniti, F., Passamonti, L., 2014. Personality traits modulate subcortical and cortical vestibular and anxiety responses to sound-evoked otolithic receptor stimulation. J. Psychosom. Res. 77, 391–400. https://doi.org/10.1016/j.jpsychores.2014.09.005
Nigro, S., Indovina, I., Riccelli, R., Chiarella, G., Petrolo, C., Lacquaniti, F., Staab, J.P., Passamonti, L., 2019. Reduced cortical folding in multi-modal vestibular regions in persistent postural perceptual dizziness. Brain Imaging Behav. 13, 798–809. https://doi.org/10.1007/s11682-018-9900-6